Cannabis Medicine as an Alternative PTSD Treatment

November 13, 2023
137 views
Cannabis shows promise as an adjunct treatment in easing PTSD symptoms, like anxiety & memory loss.
Causes and Effects of PTSD
Post-Traumatic Stress Disorder (PTSD) is characterized by the haunting grip of vivid flashbacks, intrusive thoughts or images, nightmares, and overwhelming distress caused by reminders of trauma. It can be an agonizing battle for those who experience it, sometimes leading to manifestations of physical sensations like pain, sweating, nausea or trembling. In recent years, an increasing body of research has begun to shed light on the therapeutic possibilities of cannabis for managing these harrowing symptoms. Let's examine how this healing plant may offer a glimmer of hope, whether as CBD oil for PTSD or medicinal cannabis for PTSD, for those seeking respite from the tormenting effects of PTSD.
The pathogenesis of PTSD is a multifaceted journey shaped by a complex interplay of genetic, environmental and psychological factors. Genetic predisposition can make some individuals more susceptible to developing PTSD in the face of adversity, emphasising the importance of identifying the right treatments for PTSD. Cumulative life adversities, such as early childhood trauma or repeated exposure to stressful events can sensitize an individual to the impact of traumatic incidents. The intense peri-traumatic emotional response during a traumatic event can engrave the experience deeply in an individual's memory, setting the stage for long-term distress. A lack of social support and additional life stressors can exacerbate the likelihood of developing PTSD, creating a fertile ground for its onset.
This intricate web of factors, in turn, could lead to neurochemical imbalances characterized by emotional hyper-arousal and anxiety, stressing the importance of evidence-based therapies for PTSD. These neurochemical disorders can also manifest as increased reactivity in the amygdala, the suppression of the hippocampus, and disruptions to the prefrontal cortex, contributing to hallmark symptoms and emotional turmoil that define PTSD, like attentional bias towards threats, memory fragmentation, flashbacks, severe anxiety and thought suppression. Understanding this pathogenesis is crucial for tailoring effective treatments and interventions to support individuals on their journey to recovery.
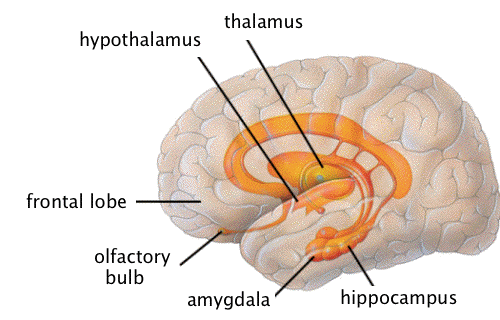
Neurocircuitry of PTSD
Let’s look a little into the neurocircuitry of PTSD. PTSD usually affects the medial prefrontal cortex, hippocampus, amygdala and hypothalamus in the brain. The medial prefrontal cortex regulates emotions and the function of the amygdala. The amygdala is the processing centre of emotions. When a PTSD patient experiences traumatic stimuli, the medial prefrontal cortex often fails to inhibit amygdala activation, resulting in fear. In other instances, overactivation of the medial prefrontal cortex due to traumatic stimuli can lead to amygdala suppression, resulting in social detachment or emotional numbness.
Limitations of Conventional Medicine
Conventional medicine's approach to treating PTSD has been marked by its limited efficacy and significant challenges, leaving an opportunity to explore alternative treatments for PTSD. Mainstream medications, such as paroxetine and sertraline, have shown only modest success in alleviating PTSD symptoms. Even more disheartening is the fact that these drugs yield full remission in less than 30% of patients, leaving the majority still grappling with their distressing symptoms. Moreover, side effects associated with these medications often lead to low patient compliance, further diminishing their overall effectiveness. This reality underscores the urgent need for alternative treatment approaches and highlights the complexity of addressing the profound and far-reaching impacts of PTSD.
While evidence-based therapies like Cognitive Behavioural Therapy (CBT), Prolonged Exposure (PE), and Eye-Movement Desensitization and Reprocessing (EMDR) have shown promise, a substantial portion of individuals with PTSD tend to avoid psychological treatments altogether. High dropout rates further underscore the limitations of these therapeutic methods. This raises critical questions about the accessibility and acceptability of conventional treatments, reinforcing the need for a more comprehensive and patient-centred approach to addressing the complexities of PTSD. Here is where the effects of cannabis on PTSD symptoms become intriguing.
The Effect of Cannabis on PTSD
Due to the shortcomings of current treatment modules, there has been increased interest in cannabis medicine as a potential therapy for PTSD. One of its notable benefits lies in its ability to assist in the extinction of traumatic memories, offering hope for individuals plagued by relentless flashbacks and intrusive recollections. Beyond that, cannabinoids have demonstrated anxiolytic and antidepressant effects. Cannabis shows potential for improved sleep as well. The potential of cannabis in PTSD therapy makes cannabinoids a valuable addition to the toolkit of treatments for individuals seeking respite from the debilitating grip of PTSD.
Research has indicated that cannabinoids – unique cannabis compounds – can effectively reduce responses to conditioned fear cues, impair the retrieval of emotionally aversive memories, and facilitate the extinction of fear-based memories. All this happens due to the relationship between the endocannabinoid system and PTSD. Additionally, a double-blind, placebo-controlled trial demonstrated that the inhibition of fatty acid amide hydrolase (FAAH), which leads to increased levels of anandamide, can enhance fear extinction and mitigate autonomic stress reactivity. These findings shed light on the potential of cannabinoids to address the core mechanisms underpinning PTSD.
The use of cannabis as a medicinal tool for managing symptoms of Post-Traumatic Stress Disorder has yielded a mix of short and long-term effects, as observed in a study of 404 medical cannabis users. In the short term, inhaled cannabis proved to be a powerful ally, reducing PTSD symptoms by more than 50%, with higher doses correlating with substantial decreases in anxiety and intrusive thoughts. However, a noteworthy aspect is the observed development of tolerance over time, as patients required increased doses to manage anxiety effectively. Intriguingly, the effects of cannabis on PTSD symptoms neither significantly improved nor exacerbated in the long run, suggesting that its long-term efficacy remains inconclusive. It is crucial to acknowledge that in our current understanding cannabis can provide immediate relief from PTSD symptoms, but appears to offer only temporary relief.
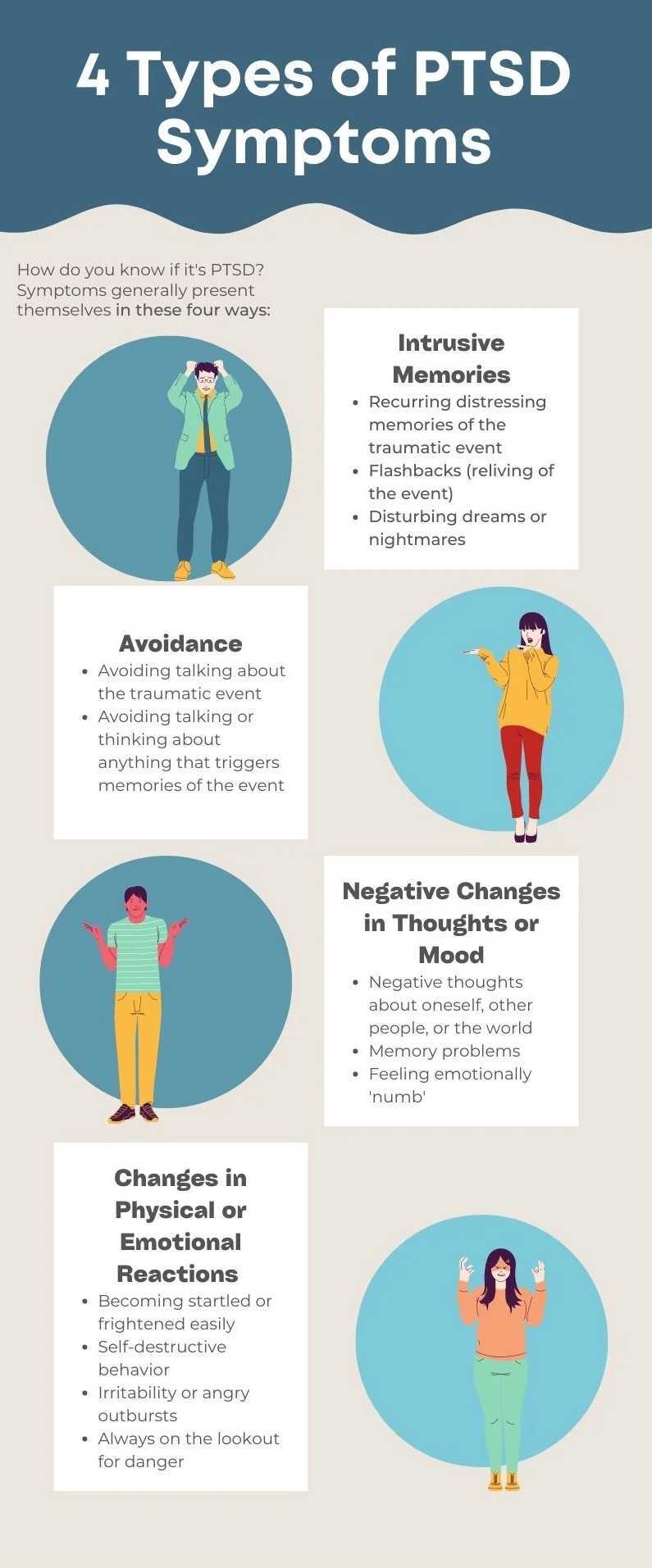
A recent systematic review examining the use of medicinal cannabis for PTSD and synthetic cannabinoids in the context of PTSD has also unveiled promising results. By acting on the endocannabinoid system (ECS), both cannabis and synthetic cannabinoids have demonstrated a potential therapeutic role in reducing PTSD symptoms. The review suggests that these compounds effectively reduce anxiety, modulate memory-related processes and improve sleep, providing a multi-faceted approach to addressing the complex symptoms of PTSD.
The potential benefits of cannabis for individuals suffering from PTSD are multi-faceted and intriguing. Emerging research suggests that phytocannabinoid medicine, by influencing various brain regions and the endocannabinoid system, may offer relief from the symptoms of PTSD, including anxiety, memory disturbances, and sleep disruptions. Its potential to modulate the amygdala and prefrontal cortex presents a compelling case for further exploration and highlights its potential as an adjunct therapy in the complex journey of managing PTSD.

