What is PCOS?



Polycystic Ovary Syndrome (PCOS) is one of the most common hormonal disorders affecting women of reproductive age and yet it’s also one of the most misunderstood.
Despite the name, PCOS is not just about “cysts in the ovaries.” It is a complex metabolic and hormonal condition that affects how the ovaries function, how the body responds to insulin and how certain hormones are produced and regulated. For many women, it shows up as irregular periods. For others, it may first appear as acne, weight gain or difficulty conceiving.
What are ovarian cysts in PCOS?
In PCOS, “cysts” are actually small, immature follicles that fail to release an egg. They are not dangerous growths, but fluid-filled sacs formed due to disrupted ovulation.
Understanding PCOS properly is the first step toward managing it effectively.
What Exactly Happens in PCOS?
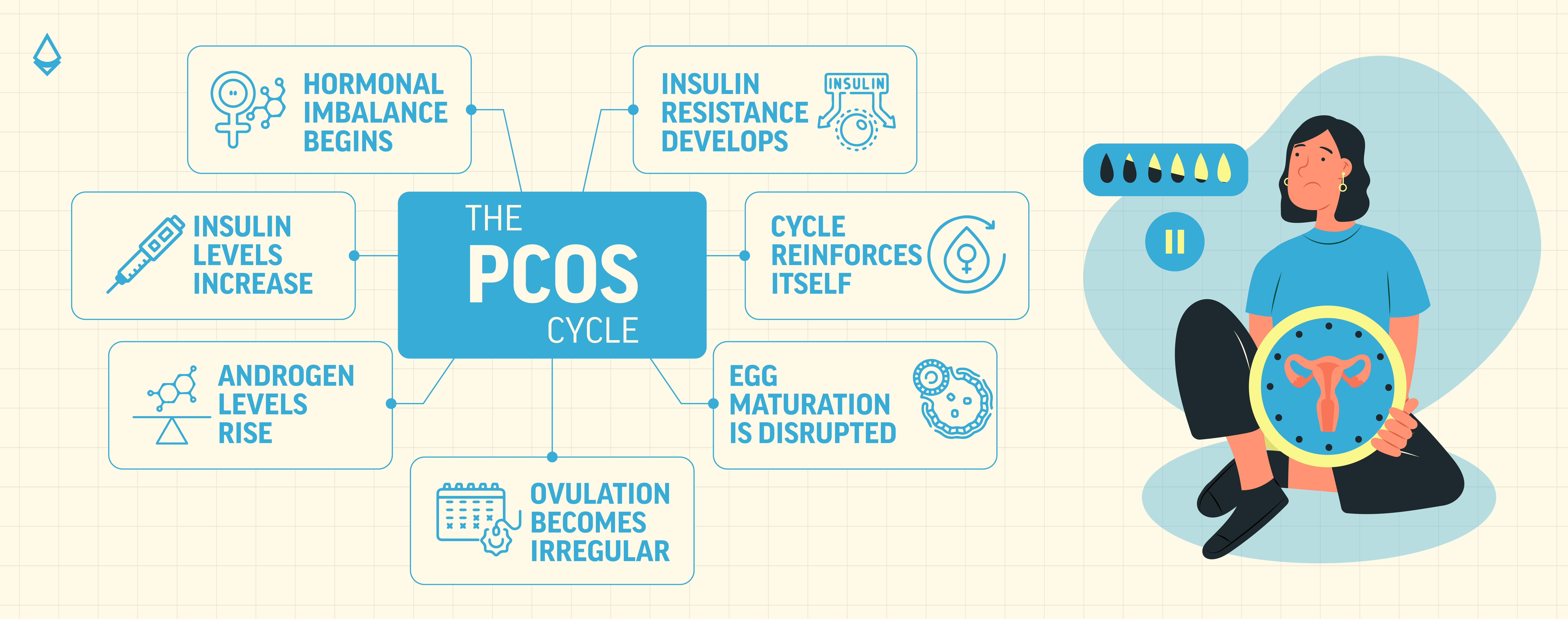
In a typical menstrual cycle, the ovaries release one mature egg each month. In PCOS, hormonal imbalance interferes with this process.
There are three main underlying features:
Irregular ovulation - The ovaries may not release an egg regularly.
Excess androgens - Higher-than-normal levels of “male” hormones like testosterone.
Insulin resistance - The body doesn’t respond efficiently to insulin, leading to higher insulin levels.
Not everyone with PCOS will have ovarian cysts. The term “polycystic” refers to the appearance of multiple small follicles seen on ultrasound; these are immature follicles, not dangerous cysts.
Common Symptoms of PCOS
Symptoms vary widely from person to person. Some women experience mild signs; others struggle with multiple issues.
The most common symptoms include:
Irregular, infrequent or missed periods
Heavy menstrual bleeding
Hirsutism
Persistent acne, especially along the jawline
Thinning hair or hair loss on the scalp
Weight gain or difficulty losing weight
Darkening of skin around the neck or underarms (a sign of insulin resistance)
Difficulty conceiving
What is hirsutism?
Hirsutism is excessive hair growth in women on areas where men typically grow hair, like the face, chest or back, often caused by higher levels of androgens.
Because symptoms overlap with other conditions, PCOS is sometimes diagnosed late, especially if periods are only mildly irregular.
What Causes PCOS?
The exact cause is not fully understood, but research points to a combination of factors:
1. Insulin Resistance
Around 60-70% of women with PCOS have some degree of insulin resistance. When insulin levels are high, the ovaries are stimulated to produce more androgens, which disrupt ovulation.
2. Hormonal Imbalance
Higher levels of luteinizing hormone (LH) and androgens interfere with normal egg maturation.
What is luteinizing hormone (LH)?
LH is a hormone that triggers ovulation and supports egg maturation in the ovaries. In PCOS, higher-than-normal LH levels can disrupt this process.
3. Genetics
PCOS often runs in families. If someone’s mother or sister has it, then the risk is higher.
4. Chronic Low-Grade Inflammation
Emerging research suggests that persistent inflammation may contribute to excess androgen production.
How is PCOS Diagnosed?
Doctors typically use the Rotterdam criteria, which require at least two of the following three features:
Irregular or absent ovulation
Clinical or biochemical signs of excess androgens
Polycystic ovaries on ultrasound
What is the Rotterdam criteria?
The Rotterdam criteria are guidelines doctors use to diagnose PCOS. A diagnosis requires at least two of these three features: irregular or absent ovulation, excess androgens or polycystic ovaries on ultrasound.
Blood tests are usually done to measure hormone levels, thyroid function, prolactin and blood sugar markers to rule out other conditions.
Because PCOS affects multiple systems, diagnosis often requires looking beyond just the ovaries.
PCOS and Fertility
Many women discover they have PCOS when trying to conceive. Irregular ovulation can make timing difficult.
However, PCOS does not mean infertility. With proper management, including cycle tracking, metabolic support and medical guidance where necessary, many women with PCOS conceive successfully.
The key is restoring more regular ovulation rather than focusing only on the ovaries.
What Are the Long-Term Health Risks of PCOS?
PCOS is not just a reproductive issue. If unmanaged, it can increase the risk of:
Type 2 diabetes
High cholesterol
High blood pressure
Sleep apnea
Endometrial hyperplasia
Anxiety and depression
What is endometrial hyperplasia?
Endometrial hyperplasia is the thickening of the uterine lining, often caused by prolonged exposure to estrogen without enough progesterone.
This is why early management is important, even if pregnancy is not a concern.
What Are Some Practical Ways to Manage PCOS?
There is no “one-size-fits-all” approach. Management focuses on improving insulin sensitivity, balancing hormones and reducing inflammation.
1. Nutrition for Insulin Balance
Prioritise protein at every meal
Include fibre-rich foods (vegetables, seeds, legumes)
Reduce ultra-processed carbohydrates
Pair carbs with protein or healthy fats to avoid blood sugar spikes
Small changes in meal timing and composition can significantly improve symptoms.
2. Strength Training Over Excessive Cardio
Resistance training improves insulin sensitivity more effectively than long hours of cardio. Muscle acts like a glucose sponge - the more it is built, the better the metabolic response becomes.
3. Stress Regulation
Chronic stress raises cortisol, which can worsen hormonal imbalance. Breathwork, restorative yoga or even slow evening walks can make a measurable difference.
4. Sleep Quality
Poor sleep worsens insulin resistance. Aim for 7-8 hours of consistent sleep.
5. Weight Management (If Needed)
Even a 5-10% reduction in body weight can improve ovulation in overweight individuals. However, not all women with PCOS are overweight; lean PCOS exists, too.
6. Supporting Inflammatory Balance
Emerging research links PCOS with chronic low-grade inflammation. Alongside diet and lifestyle changes, cannabinoids are being studied for their interaction with the body’s endocannabinoid system. When used responsibly and under professional guidance, cannabinoid-based formulations may complement lifestyle strategies aimed at supporting overall hormonal and metabolic balance.
What is the Emotional Impact of PCOS?
PCOS can affect body image, mood and self-esteem. Acne, hair growth and weight changes can be distressing. Women with PCOS have higher rates of anxiety and depression. Seeking psychological support when needed is just as important as addressing physical symptoms.
The Takeaway
PCOS is a complex hormonal and metabolic condition - not just a gynaecological issue. It affects cycles, skin, metabolism, fertility and long-term health.
The good news is that it is manageable. With early diagnosis, consistent lifestyle support and informed medical care, many women regulate their cycles, improve symptoms and protect their long-term health. Understanding our body is powerful. And with PCOS, knowledge truly changes outcomes.
Key Takeaways
- - PCOS is a hormonal and metabolic condition not just “ovarian cysts.” It affects ovulation, insulin response, and androgen levels.
- - Core drivers include irregular ovulation, excess androgens, and insulin resistance.
- - Symptoms vary widely: irregular periods, acne, hirsutism, weight changes, and difficulty conceiving are common.
- - PCOS increases long-term risks like type 2 diabetes, high cholesterol, and endometrial hyperplasia if unmanaged.
- - Lifestyle strategies — insulin-focused nutrition, strength training, sleep, and stress regulation play a central role in management.