The 4 Stages of Rheumatoid Arthritis



What Are the Four Stages of Rheumatoid Arthritis?
Rheumatoid arthritis (RA) is a chronic autoimmune disease that mistakenly causes the body’s immune system to attack healthy joint tissue. Unlike regular arthritis that results from wear and tear, RA causes inflammation in the lining of your joints, leading to pain, swelling, stiffness, and, over time, joint damage.
But RA doesn’t happen overnight. It progresses through defined stages, each with its signs, symptoms, and implications. Understanding these stages can help people with RA take early action, manage symptoms better, and preserve their quality of life.
Stage 1: Early Stage Rheumatoid Arthritis
This is the beginning of the disease, and it’s often the hardest to diagnose. The symptoms at this point can mimic many other conditions. There’s inflammation in the joint lining (synovium), but no visible joint damage on X-rays or scans yet.
What is the synovium and why is it important in rheumatoid arthritis?
The synovium is the protective lining around joints and in RA, the immune system mistakenly attacks it first, causing inflammation and swelling.
Symptoms may include:
Joint stiffness (especially in the morning)
Mild swelling
Fatigue
Occasional pain in smaller joints like fingers or wrists
Why does morning stiffness last longer in rheumatoid arthritis?
Inflammatory chemicals build up in the joints during rest, making stiffness more noticeable after waking or prolonged inactivity.
At this stage, catching RA early is key. The sooner treatment starts, the better the chances of slowing down or halting progression. Blood tests for markers like rheumatoid factor (RF) or anti-CCP antibodies, along with imaging, can help support a diagnosis.
What are anti-CCP antibodies in rheumatoid arthritis?
Anti-CCP antibodies are immune markers commonly found in RA and can help doctors detect the disease early, sometimes before severe symptoms appear.
Stage 2: Moderate Stage Rheumatoid Arthritis
In this stage, the inflammation begins to affect cartilage, which is the tissue that cushions your joints. You may start seeing visible signs of joint damage in imaging studies, even though the joints are still structurally intact.
Symptoms include:
Persistent joint pain
Swelling and warmth around joints
Reduced range of motion
Morning stiffness lasting longer than an hour
People often experience difficulty with daily tasks like gripping objects, climbing stairs, or typing. This is when joint function starts to get compromised. Treatment often includes disease-modifying antirheumatic drugs (DMARDs), lifestyle changes and possibly physical therapy to preserve mobility.
Stage 3: Severe Stage Rheumatoid Arthritis
By this point, RA is actively damaging not just the cartilage but also the bones and joint structures. The inflammation has become more aggressive, leading to deformities and functional limitations.
Symptoms include:
Visible joint deformities (such as fingers bending abnormally)
Noticeable loss of strength
Increased pain and swelling
Muscles around joints may begin to weaken or shrink (atrophy)
Why do small joints like fingers and wrists get affected first in RA?
RA commonly targets smaller joints because they contain highly active synovial tissue that is more vulnerable to immune-driven inflammation.
Stage 3 is where disability may begin to set in if the disease is not well-managed. Joint damage is often irreversible at this point, which makes ongoing care and timely intervention critical. Medications are typically more aggressive, and pain management becomes a central part of the treatment plan.
Stage 4: End-Stage Rheumatoid Arthritis
In the final stage, the joint is severely damaged, and inflammation may decrease, but this isn’t a sign of improvement. Rather, the joint has deteriorated to the point that function is significantly lost. Cartilage is gone, bones may fuse (a condition called ankylosis), and scar tissue may replace the normal joint structures.
What is ankylosis in end-stage rheumatoid arthritis?
Ankylosis occurs when damaged bones fuse together, severely restricting joint movement and flexibility.
Symptoms include:
Minimal or no joint function
Severe pain, even at rest
Stiffness that limits movement almost entirely
Potential need for joint replacement surgery or mobility aids
At this stage, quality of life is significantly affected. However, supportive therapies, assistive devices, and surgical options like joint replacement can still improve comfort and functionality.
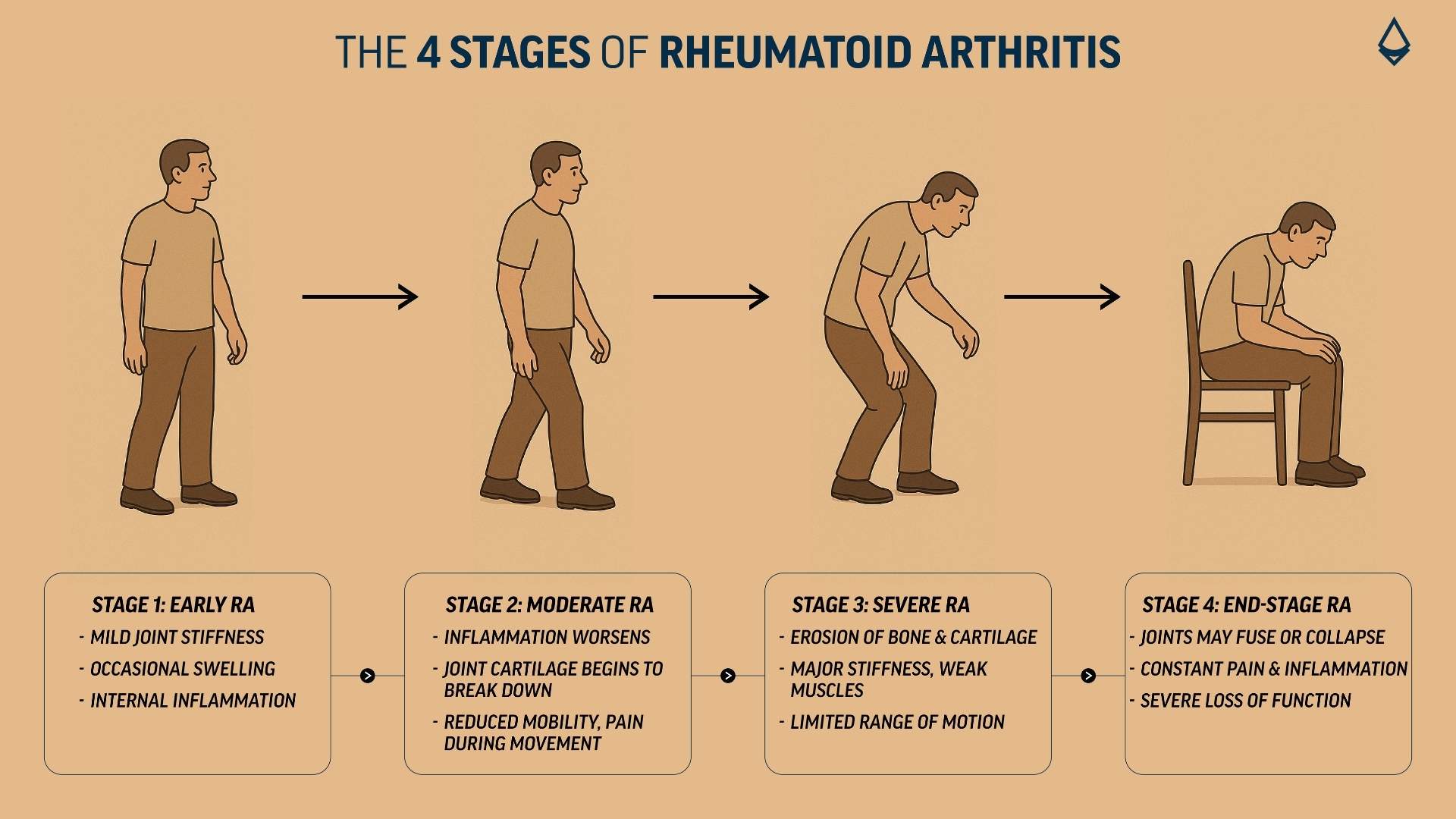
Why Understanding These Stages Matters?
RA is not a uniform disease, and its progression varies from person to person. Some people may remain in early stages for years, while others progress more rapidly. Early detection and aggressive management in Stage 1 can slow or even prevent progression to Stage 4. This includes regular monitoring, medication adherence, anti-inflammatory diets, stress management, and physical activity suited to your ability.
Cannabinoid-based medications have shown promise in managing pain, reducing inflammation, improving sleep, and supporting emotional regulation - all of which are critical in the day-to-day experience of living with RA. By interacting with the body’s endocannabinoid system, these compounds may offer a multi-targeted and gentler approach. RA may not be curable, but with the right approach, it’s absolutely manageable.
Key Takeaways
- - RA is a progressive autoimmune disease where the immune system attacks the joint lining, moving through four distinct stages of increasing severity.
- - Stage 1 is the "silent" early phase characterized by morning stiffness and fatigue; while X-rays look normal, early diagnosis here is the best chance to halt progression.
- - Stage 2 and 3 involve active physical damage, moving from cartilage erosion to visible bone deformities, which can lead to muscle weakness and significant loss of mobility.
- - Stage 4 is the end-stage where joints may fuse together (ankylosis); although inflammation may decrease, joint function is often lost, and surgery may be required.